Why heart health matters for everyone
The heart, while only the size of a clenched fist, is the powerhouse for pumping blood to all parts of your body. Due to its vital role in delivering oxygen and nutrients throughout the body, it’s critical to keep heart health at the forefront of anyone’s health journey.
Cardiovascular disease (CVD) is an umbrella term for a variety of conditions that affect the heart or blood vessels such as coronary heart disease and peripheral arterial disease. Despite many amazing advances in clinical care, CVD is still the leading cause of death for men and women, and across people of most racial and ethnic groups in the United States.1 A recent study conducted by the AHA suggests awareness that heart disease is the leading cause of death among women declined from 2009 to 2019.2
Because heart health is important for everyone, the Apple Heart and Movement Study team is beginning a series to introduce participants to the American Heart Association’s framework of Life’s Essential 8 – a set of key measures for improving and maintaining cardiovascular health that is applicable to all ages .3 This framework previously contained 7 components (“Life’s Simple 7”), specifically diet, physical activity, nicotine exposure, body mass index, blood lipids, blood glucose, and blood pressure. In the past year, however, based on an accumulating body of evidence revealing its importance, sleep health was added as an 8th component, which is what we’ll be highlighting today.
Why is sleep so important?
Sleep has become a top area of interest in both health research and the wellness space for good reason. The duration and consistency of sleep have been linked to a wide range of health topics including cardiovascular disease, metabolism, and brain health, not to mention quality of life.
Sleep duration amongst Apple Heart and Movement Study participants
Sleep health in Life’s Essential 8 is measured by duration of sleep and the American Heart Association recommends getting, on average, 7 to 9 hours per night.
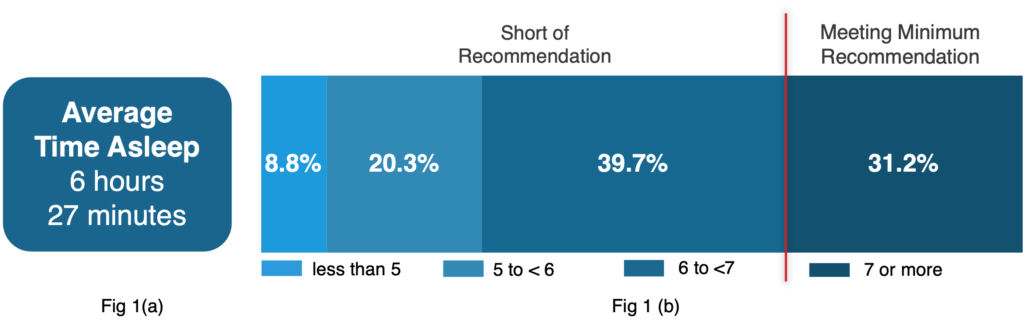
To evaluate how our Study participants compared to this recommendation, we reviewed a set of sleep measurements collected by Apple Watch over a 4-month window between February 1st, 2022 – June 1st, 2022. Of participants who were active within the Study at that time, 49.4% shared at least one night of sleep data with the Study, for a total number of over 2.9 million sleep nights shared. For simplicity, a “night” refers to the sleep period recorded, regardless of the time of day it began. For participants who had shared at least 10 nights of sleep data (a total of 42,455 participants), the average amount of time asleep per individual was 6 hours and 27 minutes. Figure 1(b) below reveals that only 31.2% met the recommended minimum of 7 hours of sleep per night.
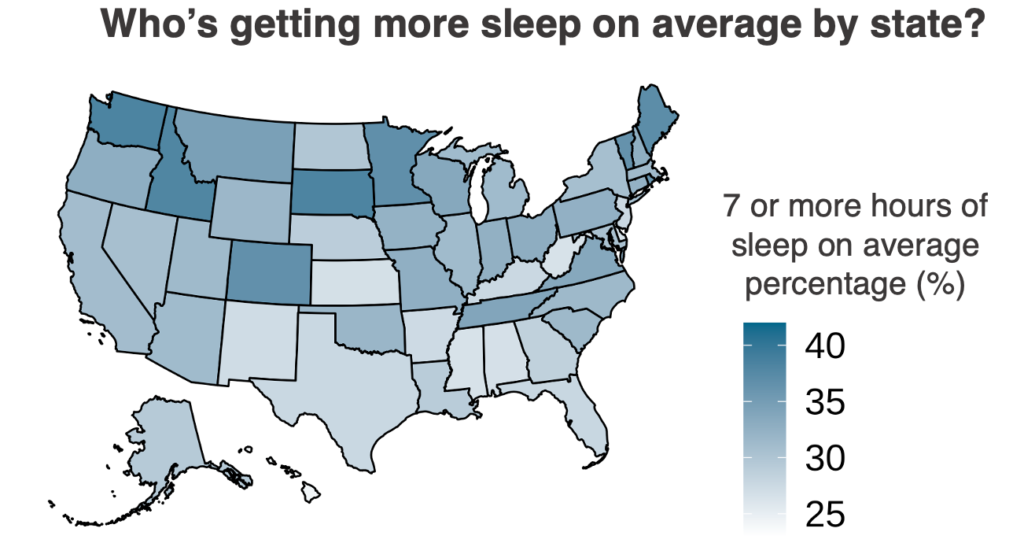
Many factors determine how people sleep, and Figure 2 shows the proportion of participants in each state averaging at least 7 average sleep hours per night. The unadjusted proportions show that Washington, South Dakota, and Idaho have the highest proportion of participants meeting the AHA’s sleep recommendation, while Hawaii, Mississippi and West Virginia have the lowest. Differences in sleep patterns between states could be related to latitude, cultural differences, demographic differences, such as age, employment status, job type (e.g., shift workers vs. farm workers), and many other factors. Despite state-level differences, in all states fewer than 40% of residents met the AHA’s recommended sleep duration.
Sleep start timing
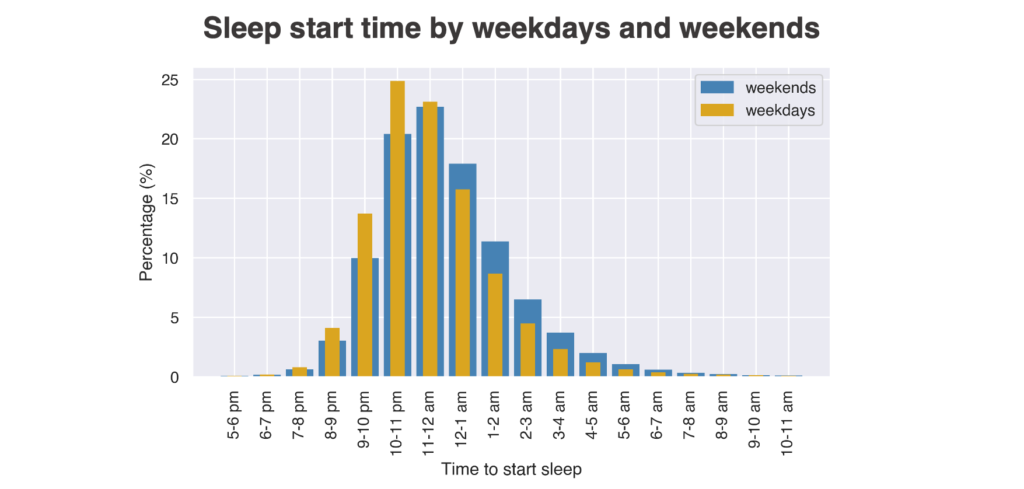
In sleep research, there is a growing interest in not only looking at total duration, but how sleep can vary, including fluctuations in how many hours of sleep a person gets per night and the variability in sleep and wake times. To start, the Study team chose to look at the differences in sleep start time for the Apple Heart and Movement Study population on weekends versus weekdays. In Figure 3 below, we show how the bedtime habits of people vary across weekdays and weekends. On weekdays, people go to bed before 12 am 66.4% of the time, but that number drops to 56.6% on weekends. This implies, as you might expect, that people tend to stay up later on weekends.
Sleep Variability
For Study participants who track and share sleep data regularly, it is also possible to explore how a variable sleep pattern may have an impact on overall health indicators and longer-term outcomes. In the figures below, we show real-world examples of sleep variability patterns for both the start time and total duration of sleep across a 29-day period with each line representing a unique participant. The blue lines represent two people with a more “regular” sleep pattern, whereas the orange lines represent two people with a more variable, “irregular” sleep pattern.
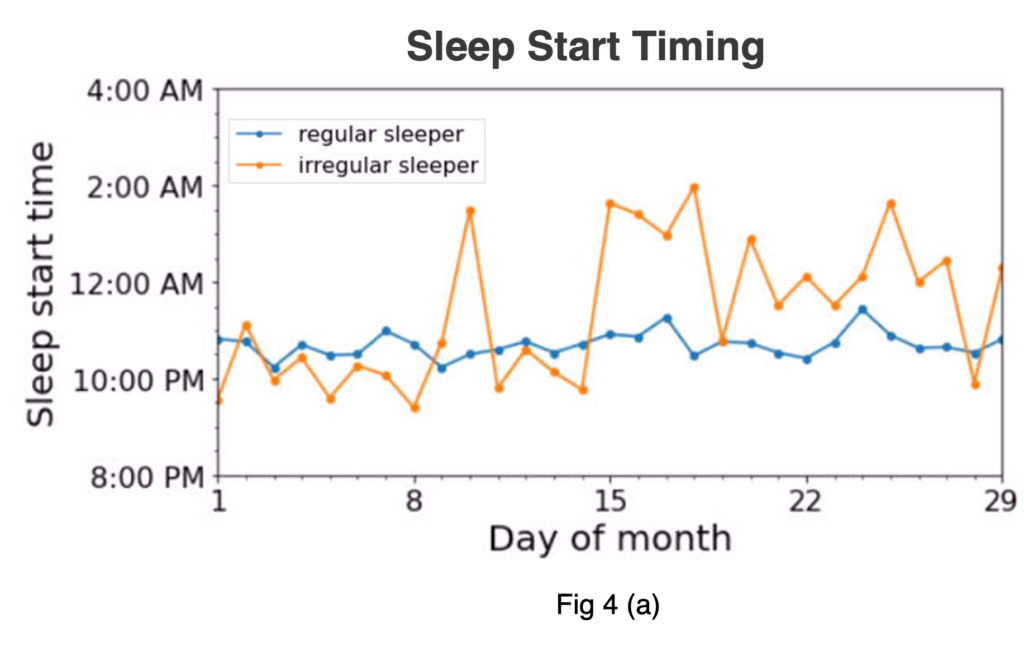
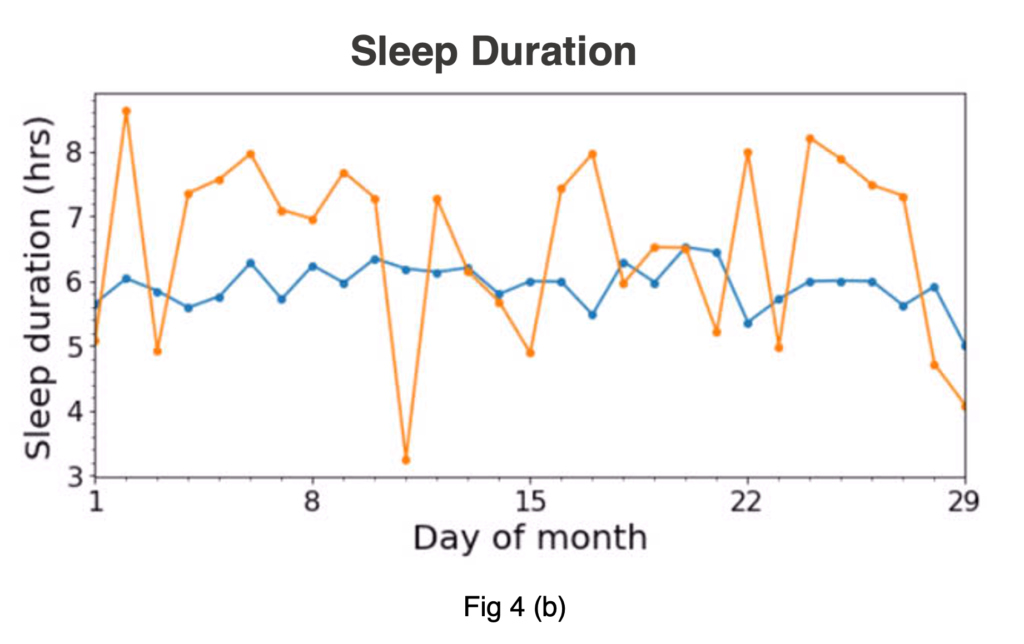
Figure 4: For demonstrative purpose only to show examples of what a sleep pattern with lower variability, or a “regular sleeper” (in blue) and higher variability, or “irregular sleeper” (in orange) can look like for both start time (a) and duration (b) across 29 days continuous days.
A recent study out of Harvard in older adults found that people with highly variable sleep patterns are more likely to have a higher BMI (body mass index), get less sleep overall, have a higher heart rate during sleep, and are more likely to show depressive symptoms, among other findings.4 The Apple Heart and Movement Study collects similar data, but in a real-world setting over a longer period of time. Initial analyses of these data suggest we’ll be able to expand upon these findings in a broader context, which we’re really excited about.
Tips for tracking sleep and improving sleep habits:
1. Measure your sleep
Past studies have shown that, in the absence of objective sleep-measuring techniques, many individuals tend to overestimate the amount of sleep they get.5 Using your Apple Watch to track your sleep is a great step towards understanding your true sleep patterns better. If you haven’t set up Sleep on Apple Watch yet and are interested in seeing your own sleep metrics, instructions to setup and view sleep data can be found here: https://support.apple.com/en-us/HT211685.
2. Establish a routine
Setting a target bedtime and routine is also important. While most daytime workers can’t sleep in, many people have greater flexibility in what time they go to bed. Establishing a target bedtime that allows you to obtain at least 7 hours of sleep and limiting screentime before bed is recommended.
With Sleep on your Apple Watch, you can set a sleep schedule and receive reminders for when to wind down. In addition, you can customize a Sleep Focus to choose what apps show on your screen and what notifications are received to limit the temptation to look at your phone and reduce the chance of disturbances.
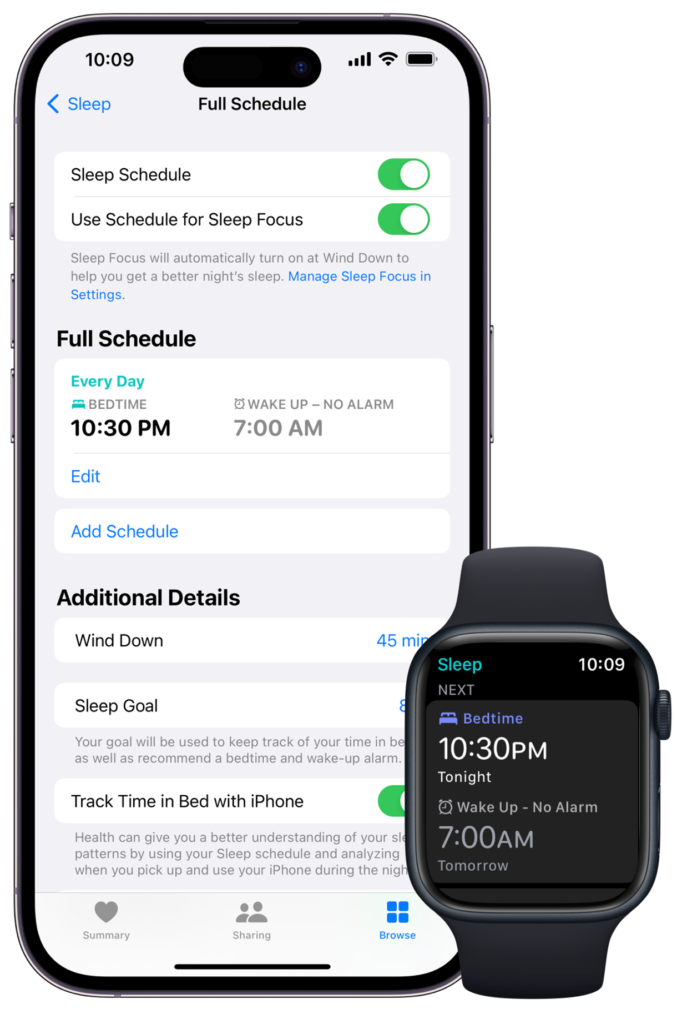
3. Consistency
While it’s not always possible to maintain a consistent sleep schedule or duration (7-9 hours), what matters, just like with exercise, is the long term. Taking steps to be more aware of your sleep patterns and learning what works best for you over time is most important.
Thank you to all our Apple Heart and Movement Study participants.
Stay tuned for Part 2 of our Life’s Essential 8 series.
Get the app. Join the Study.
- Center for Disease Control and Prevention. Heart Disease Facts. https://www.cdc.gov/heartdisease/facts.htm
- Cushman, M., Shay, C. M., Howard, V. J., Jiménez, M. C., Lewey, J., McSweeney, J. C., … & American Heart Association. (2021). Ten-year differences in women’s awareness related to coronary heart disease: results of the 2019 American Heart Association National Survey: a special report from the American Heart Association. Circulation, 143(7), e239-e248.
- Lloyd-Jones, D. M., Allen, N. B., Anderson, C. A., Black, T., Brewer, L. C., Foraker, R. E., … & American Heart Association. (2022). Life’s essential 8: updating and enhancing the American Heart Association’s construct of cardiovascular health: a presidential advisory from the American Heart Association. Circulation, 146(5), e18-e43.
- Huang, T., Mariani, S., & Redline, S. (2020). Sleep irregularity and risk of cardiovascular events: the multi-ethnic study of atherosclerosis. Journal of the American College of Cardiology, 75(9), 991-999.
- Lauderdale, D. S., Knutson, K. L., Yan, L. L., Liu, K., & Rathouz, P. J. (2008). Sleep duration: how well do self-reports reflect objective measures? The CARDIA Sleep Study. Epidemiology (Cambridge, Mass.), 19(6), 838.
Life’s Essential 8 name and mark used with permission of the American Heart Association